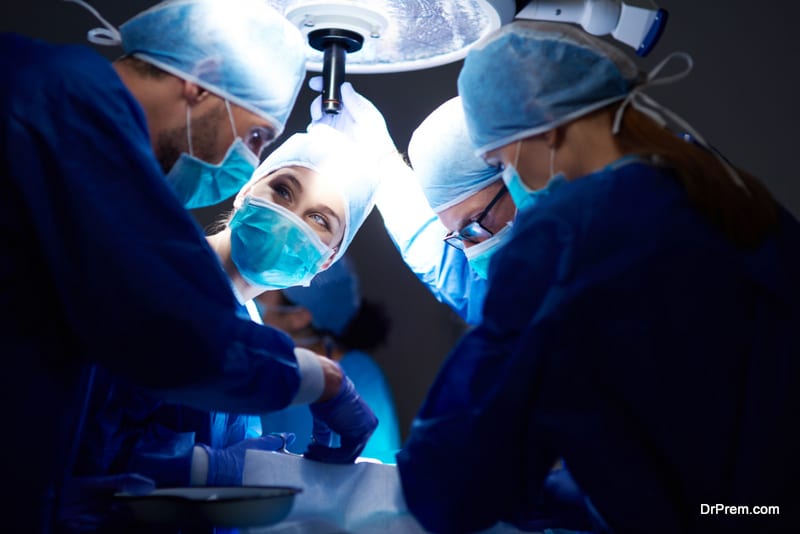
If you suddenly experience tightness in your chest, your head is spinning, your jaw clenches drastically – these are all symptoms of a heart attack. What would be your first instinct? Get me to a hospital as fast as possible. And, of course, that’s the right thing to do – get yourself in the hands of medical professionals who know how to recognize these symptoms and read the sensors they place on strategic points of your body to determine exactly what’s wrong with you.

It very well may not be a heart attack that you are experiencing, after all. It could be a pulmonary embolism, i.e. a blood clot in your lung, or just simply a pulled chest muscle – muskuloskeletal pain can be extremely intense, and can feel a lot like a heart attack, but it is not life threatening.
The important thing is that the diagnosis during this interval of extreme pain and panic for a patient should be calm, reasoned and, most importantly, accurate – so that surgical procedures are not instigated unnecessarily. And this is the case a majority of the time in our modern hospitals today – but not always.
To Operate or Not to Operate

That is the question that, like Hamlet before them, many doctors ponder with their patients, especially if they are good and thoughtful medical practitioners. But these days, with the enigma that our bloated, complicated and overwrought healthcare system has become, due to arcane legislation where everything has to come first – except the patient – the decision of whether or not to operate has wandered from strictly diagnosis into the profit-and-loss column.
A good example of this rush to operate mentality is what happens today when a high number of prostate-specific antigen (PSA) is discovered in a man’s blood test data. This may indicate prostate cancer, a noncancerous condition such as prostatitis, or simply an enlarged prostate.
The only way to determine if there is cancer for sure is via a biopsy procedure where tissue is removed from the prostate and studied. This often reveals cancerous tissue, especially in men over 50 years old. The patient is told he has cancer and that the prostate should be surgically removed or treated with radiation or hormones. But is this the best procedure for this particular patient?
Recent studies reveal that many men who are diagnosed with prostate cancer, and do not treat it, end up living long lives and die from other causes. So surgery would have been unnecessary in many instances.
But the health care system that the drug companies, hospital conglomerates, and our legislators have created does not leave much room for nuanced analysis like that. It is designed primarily to remove the cancerous part of the patient, regardless, and then relieve the effects of that surgery with pharmaceuticals. These are certainly profitable procedures but are they the best for the patient?
Surgery, No Matter How Routine, Has Risk
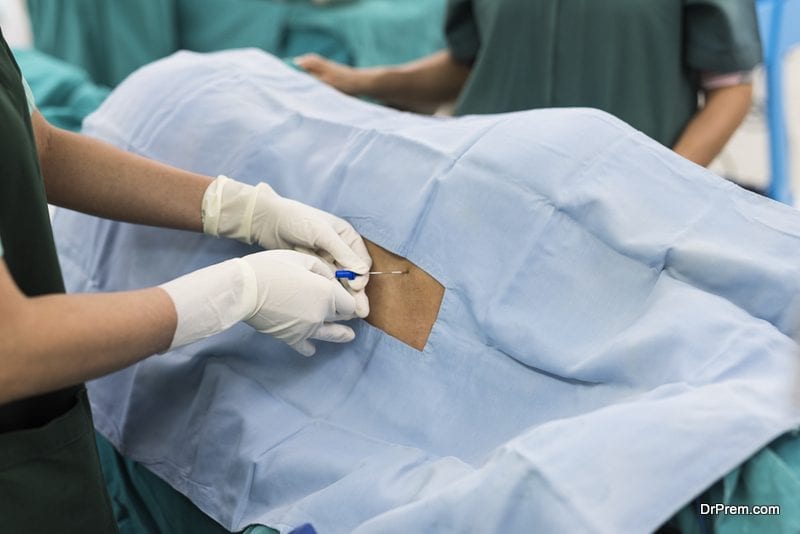 When surgery is recommended to a patient, the surgeon usually cites statistics describing the number of successful outcomes from that particular type of surgery as a percentage of all like surgeries performed. And the success rates these days are pretty high in healthy patients. But there is little talk of the bad outcomes, particularly health problems resulting from surgical mistakes during a procedure, which do happen in about 4% of surgeries, overall.
When surgery is recommended to a patient, the surgeon usually cites statistics describing the number of successful outcomes from that particular type of surgery as a percentage of all like surgeries performed. And the success rates these days are pretty high in healthy patients. But there is little talk of the bad outcomes, particularly health problems resulting from surgical mistakes during a procedure, which do happen in about 4% of surgeries, overall.
The important thing to remember is that there is always risk with any surgery. Toronto surgical errors lawyers like Gary Mazin explain it this way: “Medical malpractice that occurs during surgery can be especially hazardous to the patient’s health. Surgical errors can contribute to a host of other medical issues that may require more surgeries, longer hospital stays, and even serious consequences such as coma or death.”
So you may think you are just signing up for just the one surgical procedure, but if something goes wrong, you could be in for a long hard slog through a host of additional health issues that could last for years or even to the end of your life.
The important thing here is, make sure you get more than one opinion when faced with a surgical decision. And then discuss all the ramifications and alternative possibilities with as many experts as you possibly can before you make the commitment to go under that knife.
This decision ultimately comes down to one person – you. There will be tons of advice and huge databases available with every statistic you can think of – and you should take advantage of every single bit of that information. But when it comes down to the final decision, of whether to cut or not to cut – that decisions should be yours and yours alone.
Article Submitted By Community Writer