Often when the health effects of stress are under discussion, our thoughts will generally lean towards mental well-being. But while stress is undoubtedly a huge factor in many cases of depression, chronic anxiety and other mental health conditions, it can also affect our physical health.
Persons who are under constant stress at work will usually be more susceptible to muscle tension and back pain. However, it’s often a major contributor in the development and exacerbation of chronic illnesses too.
The role of stress in physical conditions is one which patients often underestimate; so much so, that they aren’t likely to notice how much stress is affecting them until their condition becomes much worse.
It stands to reason then that managing stress is crucial in limiting the aggravation of long-term illnesses which are already present; and also in reducing the risk of those which have not yet developed.
Here are five illnesses which have been linked to stress; and how taking measures to tackle it can help to lower the likelihood of their exacerbation.
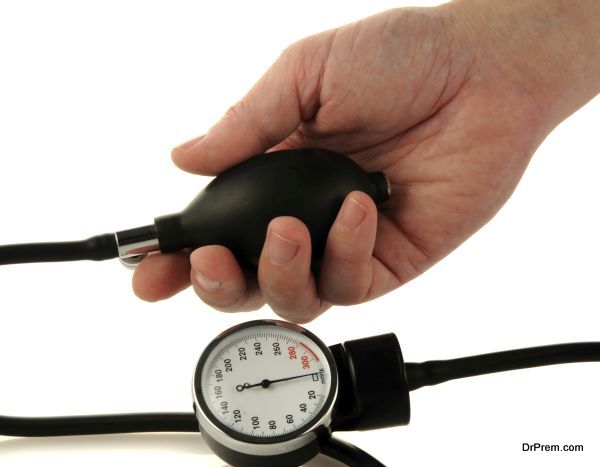
High blood pressure
Hypertension is probably the illness most commonly associated with stress in everyday conversation; and with good reason. Stress induces the release of certain hormones that can cause the heart to beat faster and in turn, bring about temporary spikes in blood pressure.
The link between stress and long-term high blood pressure however is less clear. Experts know that the two are connected, but they aren’t entirely certain how. One theory is that anxiety encourages poor lifestyle habits, which over time indirectly result in an increase in blood pressure (tobacco and alcohol use, poor dietary choices and so on). Another is that persistent short spikes in blood pressure will over time ultimately develop into chronic hypertension, due to their damaging effect on blood vessels.
The key then, is to do what you can to avoid encountering stressful situations on a recurring basis; which might appear easier said than done.
Stress reduction can be achieved through managing your workload to ease dense stretches in your schedule. But this will also necessitate taking measures not to let your work situation drive you to poor lifestyle habits outside of work.
Diabetes
One of the purposes of hormones which are released during stressful situations, including cortisol and epinephrine, is to increase the presence of sugar in the blood. This gives the body the energy boost it needs to push through the (stressful) situation it is faced with.
Those without diabetes possess the automatic capacities to counteract this, and prevent blood sugar from becoming and staying too high following high adrenaline situations. However, in those with diabetes, insulin production from the pancreas will be inhibited, meaning that the body is unable to restore normal blood sugar levels on its own during times of stress.
As a result, elevated blood sugar levels from perpetual tension can cause damage to blood vessels and increase the risk of complications, such as kidney disease, circulatory problems and organ failure.
Obviously medicines such as Victoza exist to help those with the condition keep it under control, but it’s important to remember that stress management plays a crucial role too. Those with diabetes can benefit from being able to identify what this heightened stress-hormone state feels like, and develop an awareness of their triggers. In doing so, they’ll be better equipped to avoid stress-inducing situations.
Migraine
Migraine experts have established a strong link between the onset of an attack and stress. The Migraine Trust also explains that an episode may develop in response to falling stress levels after a particularly stressful period (they refer to this as a ‘weekend migraine’).
Once more, doctors have put this down to the release of stress hormones in the body. These can cause blood vessels around the brain to swell, which induces migraine and associated symptoms.
Those who live with migraine will mostly be familiar with the treatments available and what they do. For some, mild analgesics such as paracetamol are enough to head it off in the early stages. Others might require migraine-specific treatment such as Zomig to tackle a migraine before it gets going. But if migraines are occurring on a persistent basis, such as every one to two weeks, it could well be an indication of high stress levels.
Relaxation techniques can help to lower stress levels and may in turn produce benefits in reducing the severity and frequency of migraines.
To prevent tension from building up over the course of the week to a level which necessitates a dramatic, migraine-inducing ‘comedown’ over the weekend, practising de-stressing exercises in the middle of the week, whether it’s yoga or moderate cardiovascular training, can be a useful approach.
IBS
It’s true that one of the most psychological sensitive organs in our body is the gut. When we’re anxious or going through a rough period at work or outside of it, many of us will encounter digestive problems or find ourselves going to the toilet more.
Experts once again cannot pinpoint exactly why. It might be due to the mind being more aware of gut discomfort in those who are stressed; and it could also again be a result of poor dietary choices during stressful periods.
With stress and IBS, there is also the significant issue of cyclical perpetuation. The more stressed someone becomes, the more their bowel symptoms worsen. The more their bowel symptoms worsen, the more stressed they become and so on.
Unsurprisingly, there is data to suggest that anxiety and irritable bowel syndrome are very closely linked. One study proposed that over half of those diagnosed with IBS will display characteristics consistent with one or more mental health conditions, the most prominent of which is generalised anxiety disorder (GAD).
Stress management has shown positive results in limiting the onset and severity of flare-ups in those with bowel conditions. For patients, simply liaising with a GP on a regular basis to make sure a plan is in place to help keep bowel symptoms under control helps to tackle the cyclical nature of the problem. Those with IBS should also keep in mind that stress is a prominent trigger, and set aside enough time to rest outside of work, and speak to their employer regarding their workload if they feel as though pressure is mounting.
Asthma
Clearly stress doesn’t outright cause asthma, but anxiety can be an exacerbating agent and bring about an attack. Asthma UK reports that over two thirds of those with the condition have identified stress as a trigger.
There are several reasons behind this. One is that the release of adrenaline when we’re stressed causes muscles in the airways to tense and contract, which makes airways narrower and breathing more difficult. Those who are susceptible to emotional asthma triggers may find that stress drives them to experience other feelings such as exasperation or annoyance, which can induce symptoms.
And of course, anxiety can drive us to make poor lifestyle choices (tobacco and alcohol use) which themselves may bring on asthma symptoms.
Along with the stress-management techniques already discussed above, some experts have noted that keeping a log of asthma symptoms and stressful situations can help to identify the association between them, and make it easier for patients to avoid those particular triggers.
Article Submitted By Community Writer