Multi drug-resistant tuberculosis or MDR – TB develops when tuberculosis cannot be cured even after the application of two most potent TB drugs, isoniazid (INH) and rifampicin (RMP). A promising strategy that is by targeting the outer protective covering of TB bacterium, scientists are finding new hopes in treating drug-resistant TB effectively.
 Tbfacts.Org state that about 490, 000 people worldwide have been suffering from MDR- TB in 2016 of which approximately 240,000 people died. Tuberculosis resistant to multiple drugs is a growing health menace, which has been receiving intense global attention.
Tbfacts.Org state that about 490, 000 people worldwide have been suffering from MDR- TB in 2016 of which approximately 240,000 people died. Tuberculosis resistant to multiple drugs is a growing health menace, which has been receiving intense global attention.
About 4.1% of new TB cases are MDR- TB. In 2016, an estimated 19% of already treated TB cases are either resistant to rifampicin or multiple drugs. MDR-TB treatment is harder than drug-susceptible ones requiring the use of more expensive second-line drugs dragging it over two years. By then, drugs fail to work. What is needed is to cut down on the span of treatment time and the cost.
Short span drug regimen didn’t turn out to be effective:
 The WHO in 2016 declared that about 600,000 TB cases are resistant to at least two of the commonly used front-line drugs namely, Rifampicin and Isoniazid. Not all drug-resistant TB cases are eligible for the short-span regimen. Only those resistant to rifampicin or not previously treated to the second line of drugs are considered eligible for this.
The WHO in 2016 declared that about 600,000 TB cases are resistant to at least two of the commonly used front-line drugs namely, Rifampicin and Isoniazid. Not all drug-resistant TB cases are eligible for the short-span regimen. Only those resistant to rifampicin or not previously treated to the second line of drugs are considered eligible for this.
Therefore, patient selection should be done cautiously and there should be effective patient support as well to maintain complete adherence to the program. For example, the Bangladesh Regimen ensured higher rates of remedy involving much shorter duration of about 8 to 9 months but that too did not yield effective results. Many patients experienced burning sensations that lasted for quite some time.
Overcoming challenges in treating drug-resistant TB:
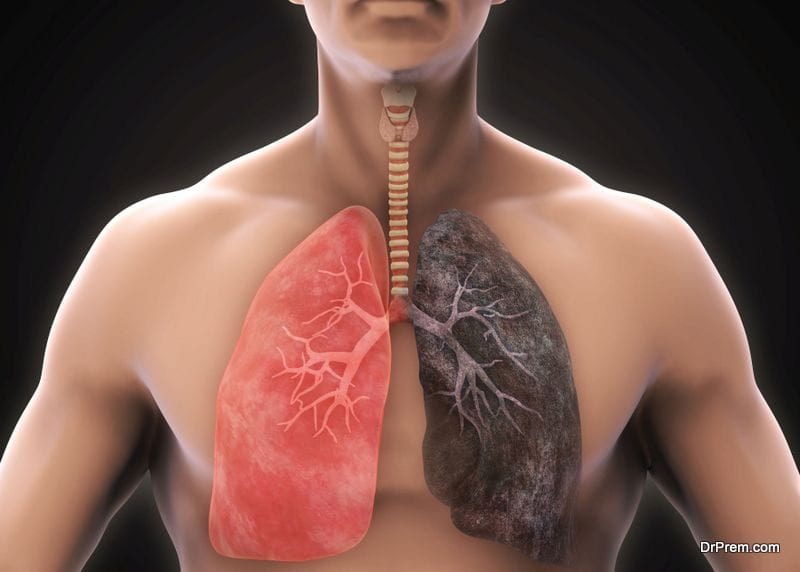 Therefore, patients with multidrug-resistant TB are left to the fate of second-line drugs which are less effective, more toxic and highly expensive. The situation is worse in poor countries owing to the unavailability of the best drugs and high treatment cost.
Therefore, patients with multidrug-resistant TB are left to the fate of second-line drugs which are less effective, more toxic and highly expensive. The situation is worse in poor countries owing to the unavailability of the best drugs and high treatment cost.
The situation is more complicated with patients having XDR-TB (Extensively drug-resistant TB). About 70% of deaths have been reported worldwide within a month of diagnosis. Diagnosis and treatment of tuberculosis resistant to multiple drugs is a major medical challenge at present.
This has always been there for many years. In 2016, Tuberculosis resistant to rifampicin (RR- TB) came under the limelight and patients infected with tuberculosis were being diagnosed by use of Gene Xpert test. This test diagnoses both types of TBs resistant to rifampicin as well as isoniazid.
Various socio-economical factors and lackadaisical attitude of the patients make this challenge insurmountable. The good news is different approaches of diagnosis and treatment have been undertaken to beat this resilient foe bringing miseries to millions of lives worldwide which are yielding. Still, it is a long way to go before this TB demon can be eradicated completely.
Newest approach in treating drug-resistant TB
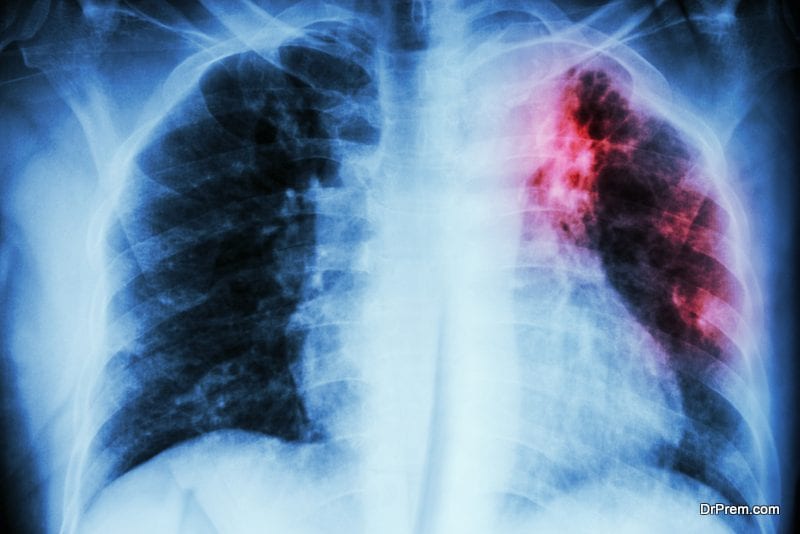 Perhaps the latest cure of treating drug-resistant TB is around the corner as revealed by the researchers from Weil Cornell Medical College in New York. In the newly published study in the journal Science and Translational Medicine, it states that disrupting the production of the waxy outer shell of TB bacterium may make it vulnerable to attack by a host of antibiotics whose effectiveness has waned off after prolonged misuse.
Perhaps the latest cure of treating drug-resistant TB is around the corner as revealed by the researchers from Weil Cornell Medical College in New York. In the newly published study in the journal Science and Translational Medicine, it states that disrupting the production of the waxy outer shell of TB bacterium may make it vulnerable to attack by a host of antibiotics whose effectiveness has waned off after prolonged misuse.
The study also highlighted another striking finding. Disruption of the fatty protective layer not only killed the bacteria but also suppressed its chances of relapse. Most importantly, it boosted the efficacy of rifampicin, the first line antibiotic drug used for TB treatment. Therefore, this approach can work well along with the application of existing drugs.
This new research seems to be highly promising as it opens a new front to create a different strategy of attack to beat this disease and ease the global TB burden. Mycobacterium tuberculosis can remain hidden inside the body undetected by our immune system. On favorable conditions, it attacks the lungs of its victim and then spread to others.
The latest sensitive TB diagnostic tests and four novel compounds to attack the bacteria in new ways have brought some hopes in treating drug-resistant TB since last decade. Latest cure mainly applies in introducing new antibiotic drugs which can fight drug-resistance else you lose the battle. The TB bacterium contains about 4000 proteins and each of them can be the potential target of new drugs.
Targeting the Bacterium’s outer waxy jacket is no doubt an innovative strategy of attacking drug-resistant TB but it will take some more years to be introduced in the market. According to Dr. Marcus Horwitz, a UCLA disease expert and a long time TB researcher, this is a no ordinary achievement.
Challenges to overcome in this new approach:
 Whether this new approach of treating drug-resistant TB would be longstanding or not is yet to be decided. Although it enhances the efficacy of the rifampicin drug, the researchers need to explore creating a new drug that would survive in the body to make a significant impact on the treatment approach.
Whether this new approach of treating drug-resistant TB would be longstanding or not is yet to be decided. Although it enhances the efficacy of the rifampicin drug, the researchers need to explore creating a new drug that would survive in the body to make a significant impact on the treatment approach.
Else the bacterium will be awakened again after the effect of rifamficin wanes off. Another key challenge would be to achieve the acceptable level of “Bioavailability”, which is vital to convert this discovery into drugs that could truly make a difference in treating drug-resistant TB.
Patient awareness is important in overcoming challenges of MDR- TB:
In view of the World Health Assembly’s global plan in 2014 to eradicate TB, newer treatment approaches need to be implemented as soon as possible but a few years wait is inevitable. In the meantime, TB patients need to be made aware of the dangerous consequences of MDR- TB guiding them properly in its prevention.
They should be strictly advised not to discontinue their medications without completing the course. Direct Observation Treatment (DOT) should be followed strictly. In case, the second-line drugs are needed, it should be done with proper expert consultation. The governments of the country should ensure a steady supply of cost-effective drugs.
The patients should be closely monitored during this phase for the adverse side effects they are likely to suffer from. If required, they may have to be kept in isolation to prevent further spread of the disease. In some cases, surgery may offer considerable benefits improving the cure rate.